Article information
Background
Vaginal cuff dehiscence following hysterectomy is considered an infrequent but potentially devastating complication. Different possible techniques for cuff closure have been proposed to reduce this threatening adverse event.
Objective
The aim of the present randomized study was to compare laparoscopic and transvaginal suture of the vaginal vault at the end of a total laparoscopic hysterectomy, in terms of incidence of vaginal dehiscence and vaginal cuff complications. Factors associated with vaginal dehiscence were also analyzed. This article presents the results of the interim analysis of the trial.
Study Design
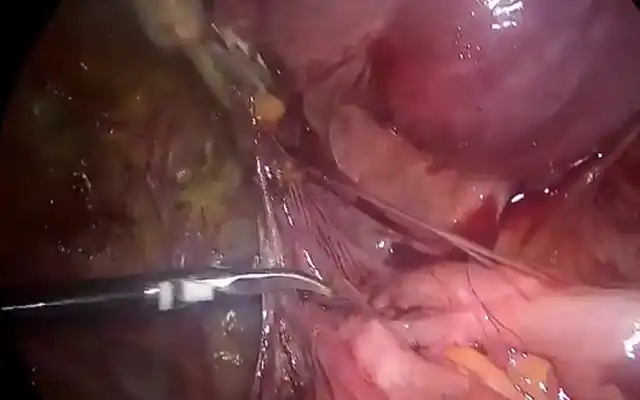
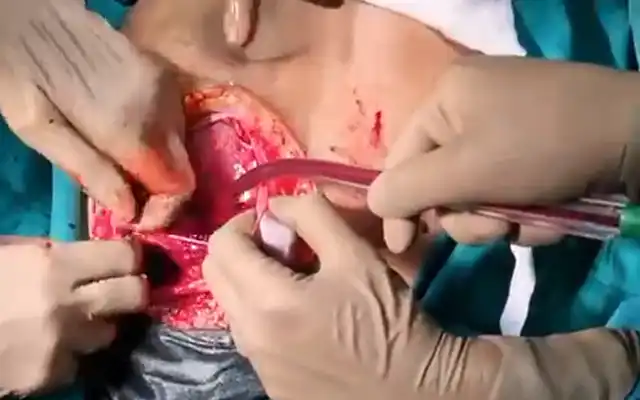
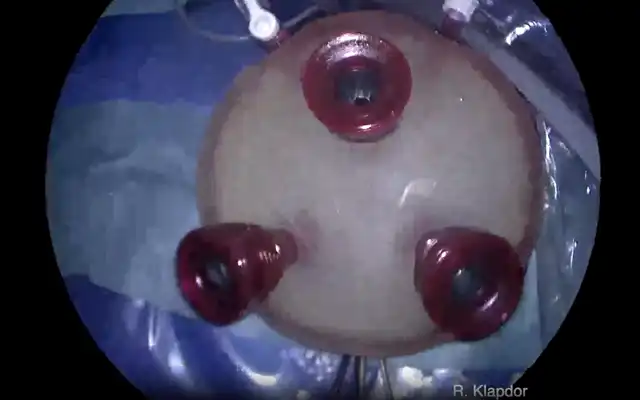
Patients undergoing total laparoscopic hysterectomy for benign indications were randomized at the time of colpotomy to receive vaginal closure through transvaginal vs laparoscopic approach using a 1:1 ratio. Allocation concealment was obtained using a password-protected randomization database. Monopolar energy for colpotomy was set at 60W. Vaginal closure was performed with a single-layer running braided and coated 0-polyglactin suture. In all cases an attempt was performed to include the posterior peritoneum in the suture. Laparoscopic knots were tied intracorporeally. All patients were scheduled for a postoperative follow-up visit 3 months after surgery, to detect possible vaginal cuff complications. Univariate and multivariable analyses were performed to identify independent predictors of vaginal cuff dehiscence after total laparoscopic hysterectomy.
Results
After enrollment of 1408 patients, a prespecified interim analysis was conducted. Thirteen (0.9%) women did not undergo the postoperative assessment and were excluded. Baseline characteristics of the 1395 patients included (695 in the transvaginal group and 700 in the laparoscopic group) were similar between groups. Patients in the transvaginal group had a significantly higher incidence of vaginal dehiscence (2.7% vs 1%; odds ratio, 2.78; 95% confidence interval, 1.16–6.63; P = .01) and of any cuff complication (9.8% vs 4.7%; odds ratio, 2.19; 95% confidence interval, 1.43–3.37; P = .0003). Based on these findings, the data monitoring committee recommended that the trial be terminated early. After multivariable analysis, transvaginal closure of the vault was independently associated with a higher incidence of vaginal dehiscence and any vaginal complication; premenopausal status and smoking habit were independently associated with a higher risk of dehiscence.
Conclusion
Laparoscopic closure of the vaginal cuff at the end of total laparoscopic hysterectomy is associated with a significant reduction of vaginal dehiscence, any cuff complication, vaginal bleeding, vaginal cuff hematoma, postoperative infection, need for vaginal resuture, and reintervention.