Authors / metadata
DOI: 10.36205/trocarvid4.2021001
Abstract
Study Objective: To confirm the validity of the Shaver technique in the treatment of postsurgical synechiae. Design: Description of the surgical steps and prognosis according to a case report Setting: “SELEC Sino European Life Expert Centre” of Jiao Tong University, Shanghai.
Case report
Patient: A 23 year old woman with a previous history of 3 D&C for induced abortions and two years of hypomenorrhea. 2/3D. Ultrasound in her early prolipherative phase showed a synechia inside the uterine cavity with an endometrial thickness of 3 mm. A fibrotic synechia in the fundal area of the uterine cavity was confirmed by diagnostic hysteroscopy with Campo Trophy – scope. Due to the patient’s desire of pregnancy, an operative hysteroscopy with a tubal patency test was planned.
Intervention
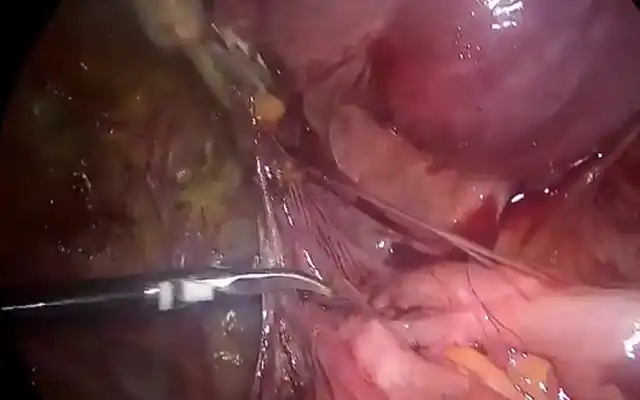
The operative hysteroscopy was performed with the Intrauterine Bigatti Shaver (IBS®) along with the use of scissor, Shaver blade and bipolar probe. The Shaver 24Fr optical system with SA blade was used. The rotational speed of the blade was 2100 rotatons pro minute (rpm) with a suction flow of 250 ml per minute. Initially, the 4 mm scissors, introduced through the IBS® strait operative channel, were used to cut the fibrotic synechia. Then, the Shaver SA blade removed the fibrotic tissue previously cut to restore the normal volume of the uterine cavity. The bipolar probe was used at the end of the procedure to control the bleeding. Finally, hydrotubation with methylene blue introduced inside both tubal ostia with a transparent silicon catheter was performed. The whole procedure lasted 6 minutes with a saline fluid deficit of approximately 300 ml. No intraoperative complications were observed, and the patient was discharged from the hospital 1 hour after the operation. The patient took Oestradiol Tablets (1mg) and Dydrogesterone Tablets (1mg) for 14 days after the operation and no antibiotic was administrated. Materegen gel by Bioregen was inserted under visual supervision inside the uterine cavity for adhesion prevention.
Main result
At one month follow up, during the patient’s early prolipherative phase, a diagnostic hysteroscopy with a Campo trophy scope was performed. The patient’s periods were regular. The uterine cavity returned to its normal shape and volume with regular endometrium and without any postsurgical adhesion.
Conclusion
This case report shows that combination of the Shaver technique with gel application for postsurgical adhesion prevention should be the treatment of choice in case of synechiae or Asherman syndrome. The Shaver technique, the aim of which is not only to cut but also to remove the fibrotic tissue, combined with the gel application should improve the results of Operative hysteroscopy. The mechanical action of the Shaver without any electrosurgery is probably the reason of the promising results in this video. The Shaver optics with the bipolar probe offers a precise coagulation under direct visual control only of the vessels involved in bleeding.