Authors / metadata
DOI: 10.36205/trocar1.2021006
Abstract
Iniencephaly is a rare neural tube defect characterized by extreme retroflexion of the head with absence of the neck due to spinal deformities. On antenatal ultrasonography, features that clinch the diagnosis of iniencephaly include deficit of occipital bone with an enlarged foramen magnum, fusion of malformed cervical and thoracic vertebrae, and upward turned face with chin being continuous with the chest because of absence of neck. Differential diagnoses include anencephaly with spinal retroflexion, Klippel-Fiel syndrome, nuchal tumours (e.g. teratoma, goitre, and lymphangioma), and Jarcho-Levin syndrome. We present a case of antenatal diagnosis iniencephaly apertus with discussion of the ultrasound features and postnatal clinical and radiological correlation.
Corresponding author: Dr Meenu Agarwal e-mail: drmeenuagarwal1@gmail.com
Introduction
Iniencephaly is a rare birth defect characterised by the triad of fixed retroflexion of head, variable degrees of cervical lordosis and dysraphism, and an occipital bone defect involving the foramen magnum.[1] Two types have been described based on the associated presence or absence of encephalocele: Iniencephaly apertus and Iniencephaly clauses, respectively.[2] Although, considered by many as invariably lethal, there are at least 8 case reports describing long-term survivals with less severe forms of disease.[3] Herein, we describe antenatal ultrasound findings in a case of iniencephaly apertus.
Case report
A 33-year-old multigravida woman visited our obstetric outpatient department for routine obstetric consultation at 15 weeks of gestation. She had neither had prior antenatal check- up nor any folic acid supplementation. She had been a hypothyroid for 4 years and was on thyroxine supplementation (50 mcg once daily). There was no h/o consanguinity. There was no history of teratogen exposure.
Patient’s obstetric history was G6P1A4L1. First pregnancy had delivered full-term, low birth weight, male child weighing 1.75 kg. Second pregnancy required medical termination of pregnancy (MTP) because of intrauterine foetal demise. Third, fourth and fifth pregnancies had ended in spontaneous abortions at 6-, 6- and 7-weeks gestation, respectively. However, she had never undergone evaluation mainly because of financial issues.
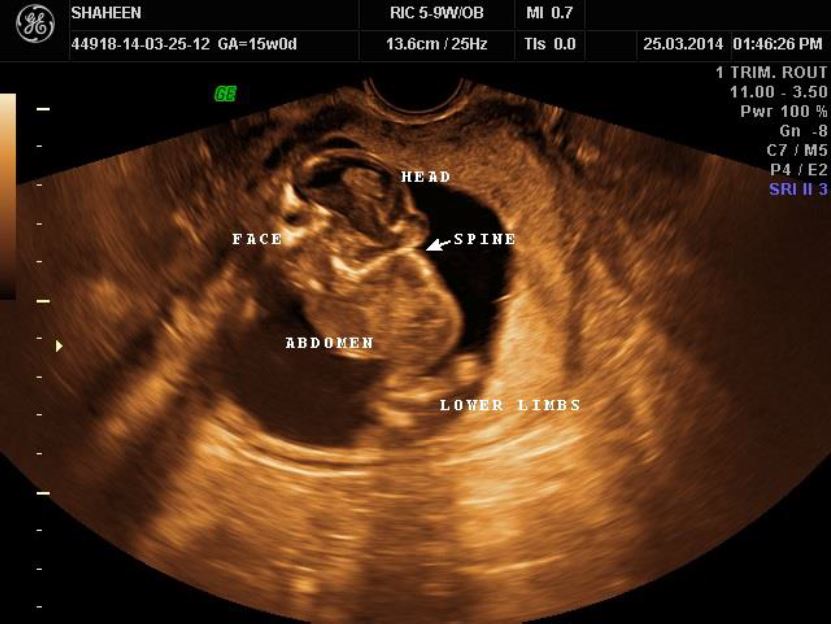
Her blood group was A-positive. Laboratory tests including complete blood picture, blood sugar, urinalysis, HIV, HBsAg and VDRL were normal. She was euthyroid with high-normal serum TSH level (3.0 mIU/L). Positive serum titres of IgG against toxoplasma and rubella were found. Ultrasonography was performed (GE Voluson using broad band 2-5 MHz convex transducer and 4-8 MHz convex volume transducer). Gray scale scan revealed foetal intrauterine growth retardation. Neck was short and hyper-extended with fixed spinal retroflexion (Figure 1).
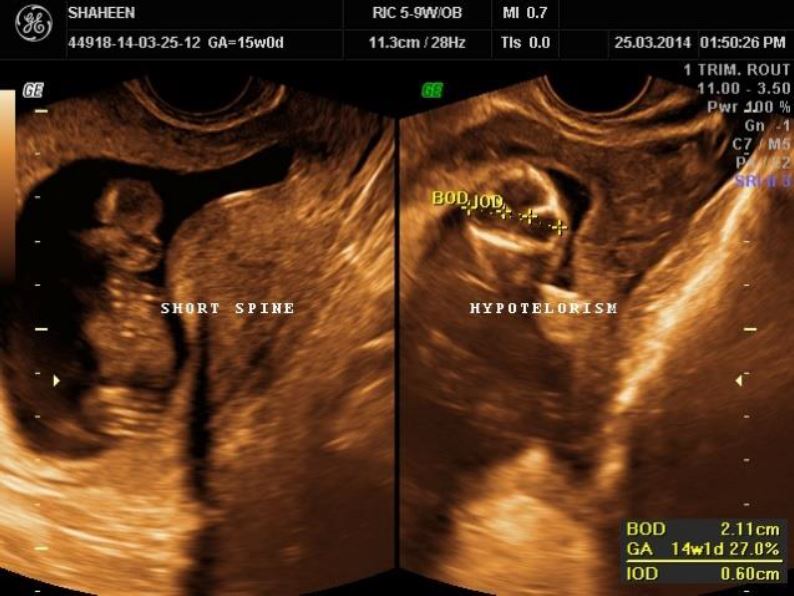
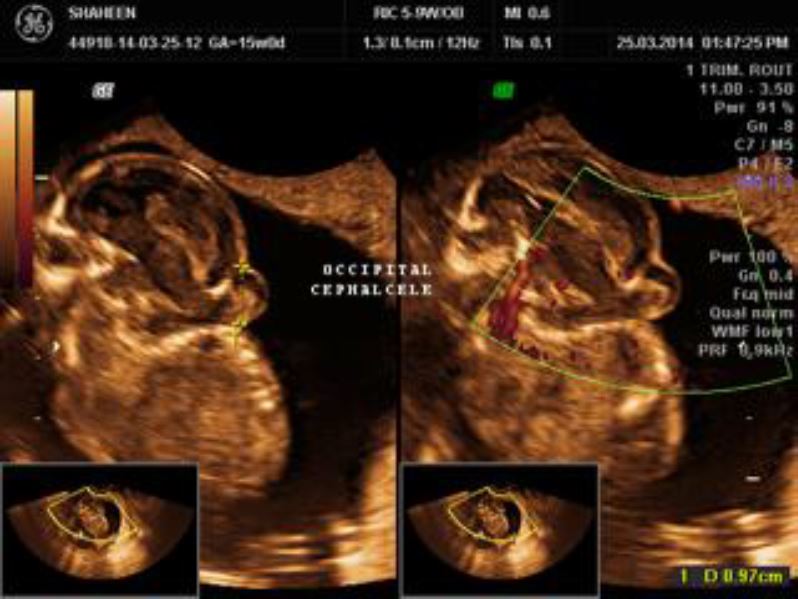
There was fusion of upper cervical vertebrae with the occiput, along with approximately 10 mm occipital encephalocele (Figure 2). Spine was very short, and lower thoracic and lumbosacral vertebrae could not be visualized indicating complete rachischisis (Figure 3).
Facial profile appeared abnormal with hypotelorism. Hands and feet appeared normal. However, the foetus did not demonstrate any limb activity during the examination period of 30 min with possible foetal akinesia. An antenatal diagnosis of iniencephaly apertus was made. In view of obvious foetal anomalies incompatible with extra-uterine life, the parents were counselled for MTP. No further specific imaging or testing was done. After giving consent, patient underwent MTP.
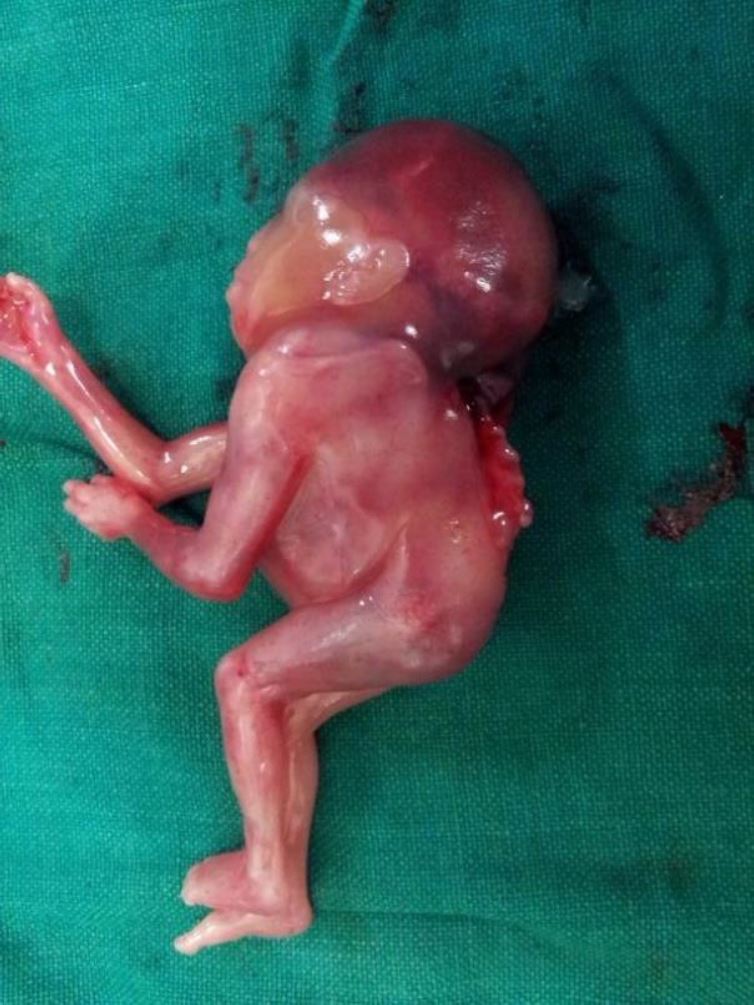
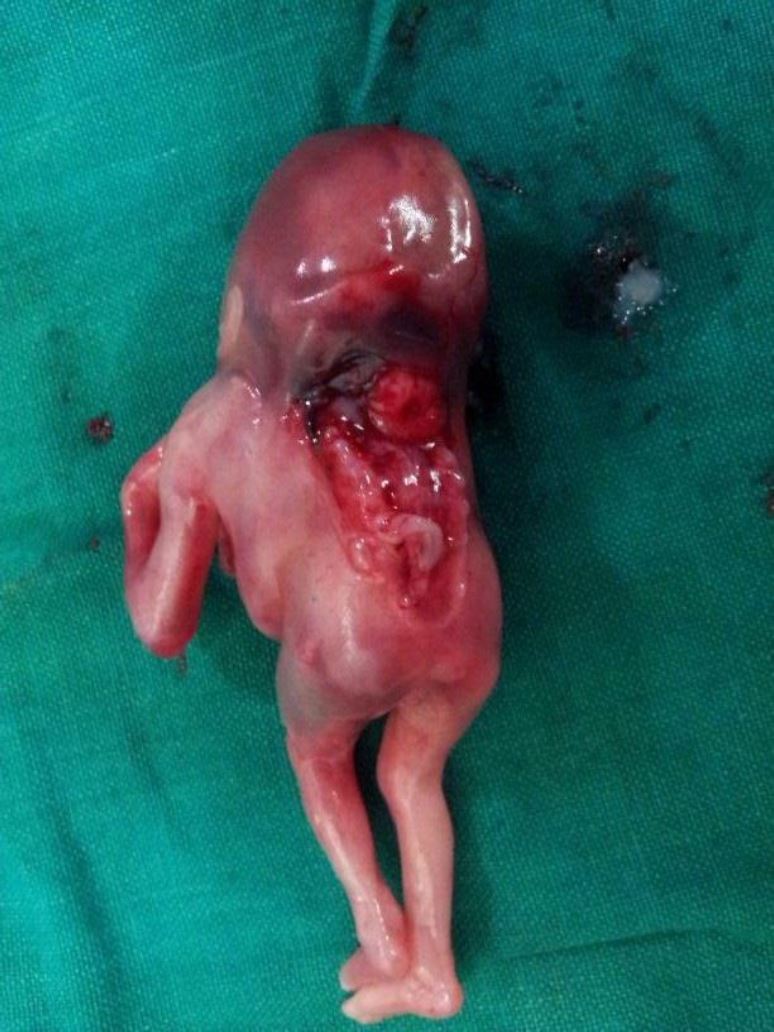
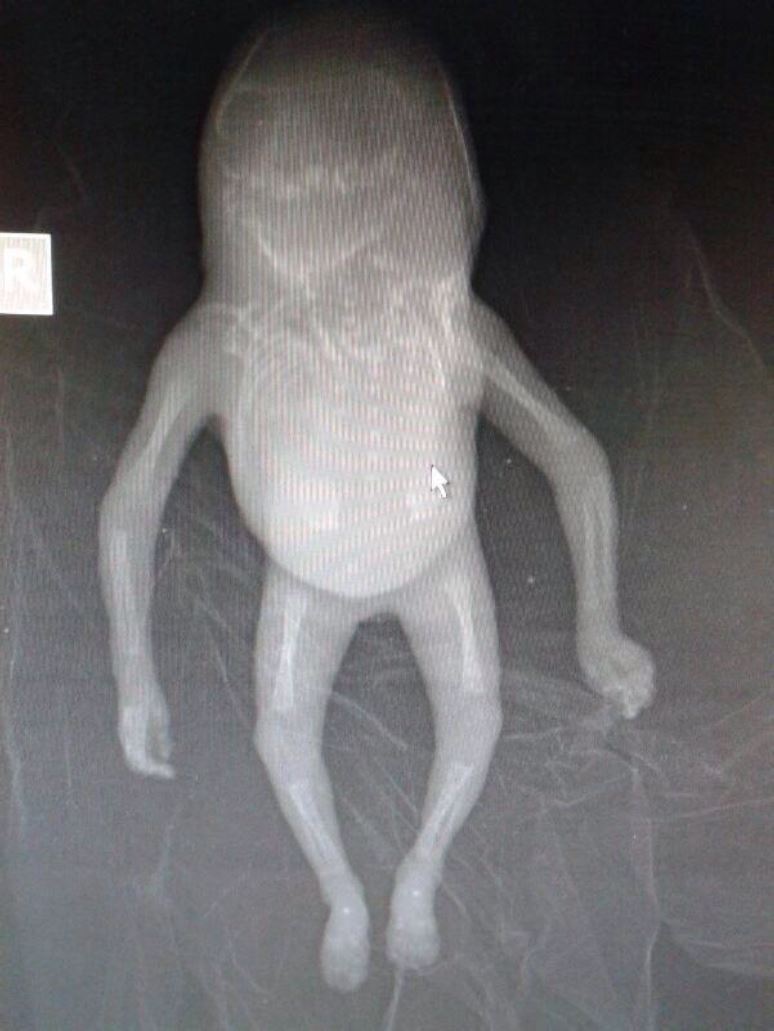
Examination of the abortus revealed a dead female foetus weighing 32 g. Antenatal USG findings of occipital encephalocele, retroflexion of head (Figure4), and rachischisis (Figure 5) were grossly confirmed. Radiograph (fetogram) showed an abnormal short spine with hemivertebrae and open spinal defect (Figure 6). The limb bones were normal. Karyotype analysis revealed normal chromosomal pattern.
Discussion
Iniencephaly is an uncommon neural tube defect (NTD). The word ‘inien’ is derived from the Greek word ‘inion’ which means nape of neck. The defective ‘inion’ (posterior most part of occipital bone) fuses with the back resulting in absence of neck and fixed retroflexion of head.4 Incidence in India is estimated to be 1 in 65,000 deliveries.[5] Overall reported incidence is higher and ranges from 0.1 to 10 in 10,000 deliveries.[6] Majority of cases are females (90%) 5 as was our case. The exact etiology and pathogenesis is unknown. Environmental factors that increase the risk of NTDs in foetus include poor socioeconomic conditions, low parity, lack of folic acid supplementation, obesity and drugs including sulphonamide, tetracycline, antihistamines and antitumor agents.[7] Iniencephaly has been reported in association with few chromosomal abnormalities including trisomy 18, trisomy 13, and monosomy X.2 Environmental factors like maternal syphilis and drugs like clomiphene citrate and sedatives have been also implicated in causation of iniencephaly.[6] However, no definite evidence exists in favour of any specific genetic and/or environmental factors being the cause (s) of iniencephaly in particular.
In our case, poor nutrition and lack of folic acid supplementation during pregnancy may be the risk factors. Further, the patient was suffering from hypothyroidism with long-term history of thyroxin intake. Also, she was tested positive for IgG against toxoplasma and rubella, which indicates prior infection. However, we could not find any established evidence of association between these factors and risk of iniencephaly.
Antenatal diagnosis of iniencephaly mainly relies on USG, and/or magnetic resonance imaging (MRI).[8] Although, in most cases a reliable diagnosis can be made on USG alone, MRI might help in cases of suspicious but atypical findings on USG. On USG, the characteristic appearance of iniencephaly has been described as a ‘star-gazing foetus’. Other features that help in the diagnosis include:
- Occipital bone deficit leading to enlarged foramen magnum without (iniencephaly clausus) or with encephalocele (iniencephaly apertus)
- Irregular fusion of malformed vertebrae
- Incomplete closure of vertebral arches and bodies
- Retroflexion of the cervical spine
- Upward turned face with chin continuous with chest because of the absence of neck
Our case had all these features, and thus, was diagnosed as iniencephaly apertus. Iniencephaly apertus should be differentiated from anencephaly with retroflexion of spine. Anencephaly shows a total or partial absence of neurocranium and retroflexed head is not covered with skin. However, in iniencephaly the retroflexed head is completely covered with skin. Cervical vertebrae are abnormal in iniencephaly, but almost normal in anencephaly. In the present case the retroflexed head was completely covered with skin and there was no encephalocele.
Iniencephaly carries bad prognosis, with the classic malformation-complex being incompatible with extra-uterine life. However, few instances of long-term survival have been reported in cases of lesser severity of iniencephaly & associated malformations.
Sources / references
Figure 1: On ultrasound scan, Fetus could be described as “stargazer” with upturned face, deficient short spine with hyperextended neck and fixed spinal retroflexion.
Figure 2: There was fused occiput with upper cervical region and a 10 mm occipital encephalocele suggesting Iniencephaly Apertus
Figure 3: The cervical and thoracolumbosacral spine was short, deficient and vertebrae could not be clearly differentiated with deficient overlying soft tissues/skin- Complete Rachischisis
Figure: 4
Figure: 5 The antenatal findings were seen in the gross postnatal fetus on examination in lateral position, figure 4 – in prone position 5
Figure: 6 Radiograph (Fetogram) revealed abnormal undifferentiated deficient vertebrae from cervical to sacral region.