Authors / metadata
DOI : 10.36205/trocar3.2023007
Abstract
Uterine malformations are defined as deviations from the normal anatomy resulting from embryological maldevelopment of the Mullerian ducts (1). The prevalence of a uterine malformation is estimated to be 24.5% in patients who experienced miscarriage and infertility (2). Hysteroscopic metroplasty is currently considered the first-choice surgical therapy (3). Several studies reported that metroplasty increased the delivery rate and reduced the risk of spontaneous abortion (4, 5, 6, 7). However, due to the lack of randomized control studies, these results are still debatable. A recent randomized control study by Rikken et al. (8) reported that septum resection did not improve the reproductive outcome. Unfortunately, due to small trial size this result could not be confirmed. In literature there has been a wide agreement to perform hysteroscopic metroplasty in patients with two previous spontaneous abortions and no other cause for pregnancy loss (9). Cararach et al. (10,11) reported a better reproductive outcome in metroplasty performed with scissors compared to resectoscopy. Duffy et al. (12) speculated that the vascular damage resulting from electricity induced thermal damage could impair uniform endometrial healing over the resected area. Our proposed technique, by using mechanical energy via scissors and Shaver to completely remove the septum, aims to improve the quality of the result and to reduce the risk of complications.
Study objective
To assess the efficacy of the surgical treatment for a complete septum (Class U2b) removal with a combined technique: “Shaver and scissors”.
Design
Description of the surgical steps and prognosis related to this new approach.
Setting
“SELEC Sino European Life Expert Centre” of Jiao Tong University, Shanghai.
Patient
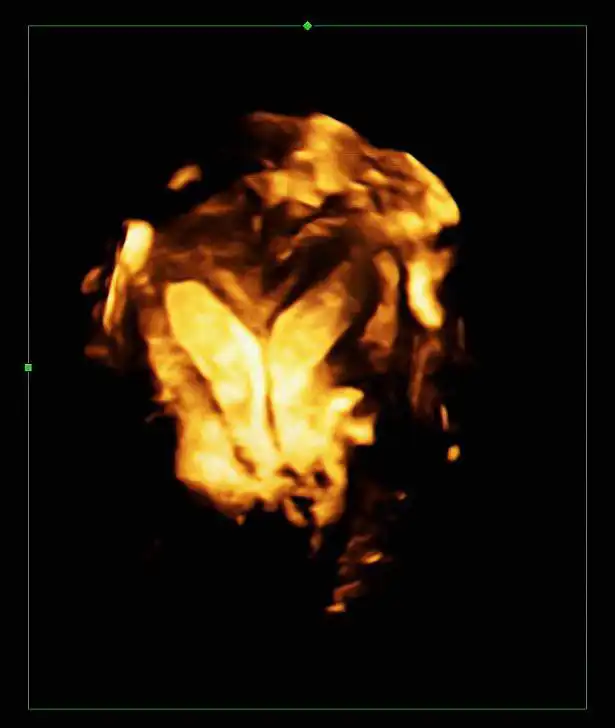
Our patient was a 31-year-old woman, 0-0-2-0, with a previous history of two first trimester miscarriages in the last two years. A 3D transvaginal ultrasound showed the presence of a complete septate uterus (U2b – ESHRE/ESGE classification) confirmed by diagnostic hysteroscopy (13). The uterine cavity was divided by a septum up to the level of the internal cervical ostium.
The histological exam showed the presence of a benign polypoid simple hyperplastic endometrium. A new combined hysteroscopic approach to correct the uterine malformation with the Shaver technique and scissors was performed. One month after metroplasty a diagnostic hysteroscopy was planned in the first half of the menstrual cycle to evaluate the completeness of our surgical approach.
Intervention
The operative hysteroscopy was performed with the Intrauterine Bigatti Shaver (IBS®) (KARL STORZ SE & Co. KG). The 24 Fr Shaver optical system (KARL STORZ SE & Co. KG) with the flute beak SB blade (KARL STORZ SE & Co. KG) was used (14). The rotational speed of the blade was set between 1500 and 2100 rotations per minute (rpm) with a suction flow of 250 ml per minute.
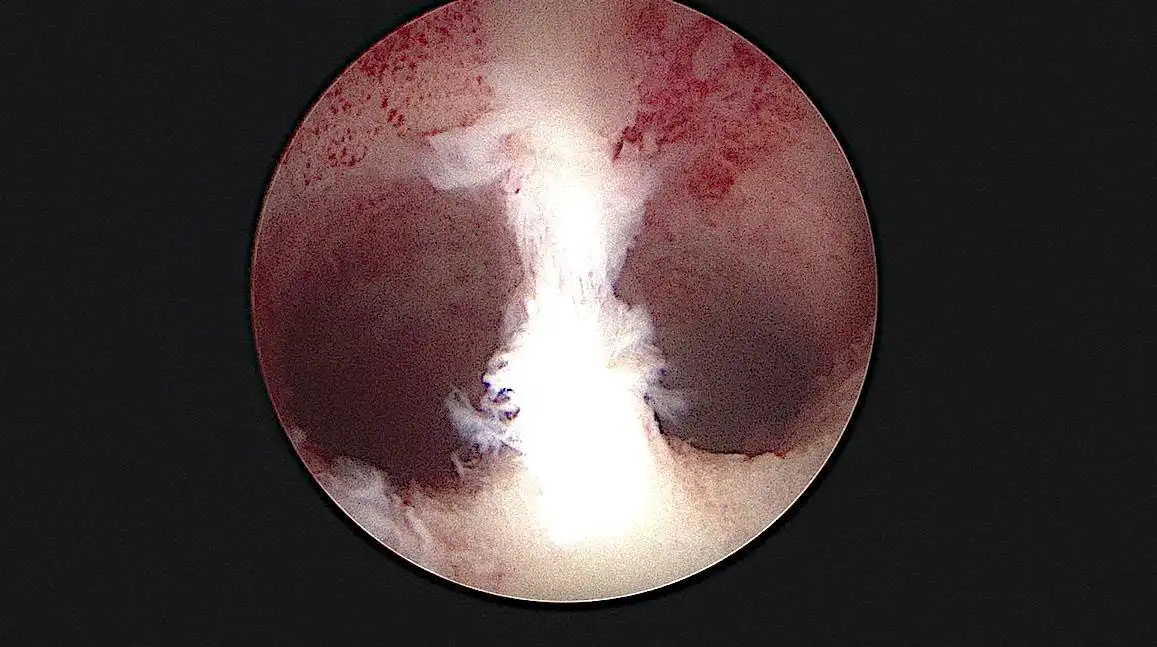
As reported during the diagnostic hysteroscopy, a complete septum with a simple hyperplastic polypoid endometrium was present in the uterine cavity. During the first step of the procedure the SB blade with a rotational speed of 2100 rpm was used to completely remove all the polypoid endometrium from both cavities.
This action reduced all the endometrial overgrowth improving the septum view.
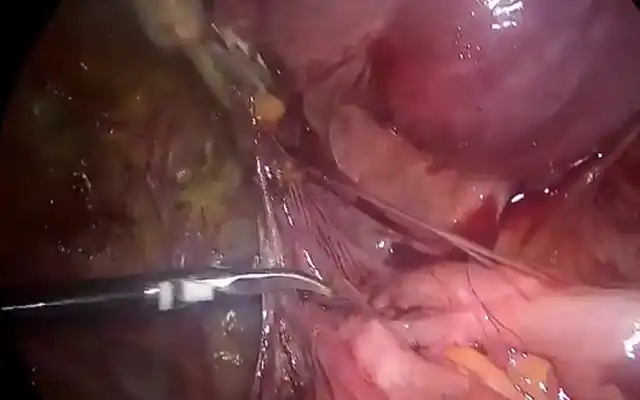
Second, scissors were used to completely dissect the septum up to the uterine fundus. For the third and final step, the Shaver SB blade was used to completely remove the upper and lower septum remining and to completely restore the volume of uterine cavity. To remove the residual septa rough edges left attached to the anterior and posterior wall, the Shaver Blade rotational speed was reduced to 1500 rpm. A perfect clear visual field was maintained during the whole procedure, and no bleeding was reported. The operative hysteroscopy lasted almost 10 minutes without any intraoperative complications. To prevent adhesion formation a Mate-Regen® by Bioregen was left in place at the end of the procedure. The patient was discharged from the hospital two hours after the operation.
Main result
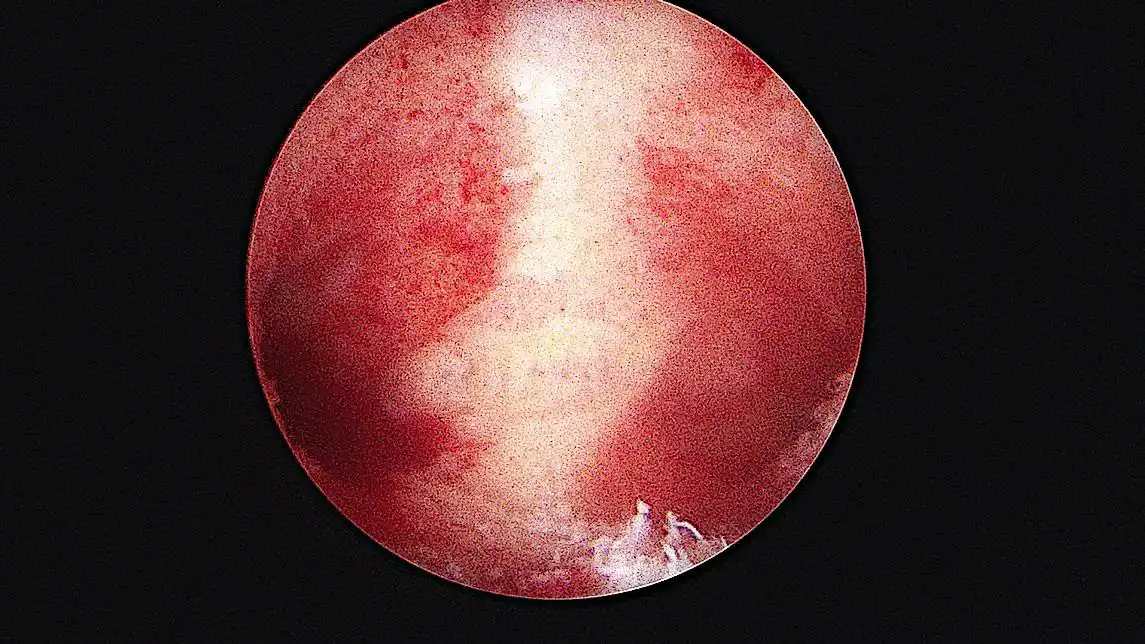
The histological exam after the metroplasty confirmed the presence of a benign simple polypoid hyperplastic endometrium. A diagnostic hysteroscopy performed during the patient’s follow up appointment three months after the operation, showed a normal uterine cavity without any remnant of the residual septa and a healthy, adhesion-free, regular proliferative endometrium.
Video
Conclusion
Presently the Shaver technique has been widely used in the treatment of all kinds of intrauterine pathologies (15). Polyps, adhesions, placental remnants, adenomyosis and all types of myoma up to 3.5 cm have been completely and safely removed with this new technique (16,17). The major advantage of mechanical tissue removal systems is their ability to remove only the functional layer of the endometrium without affecting the basal layer.
This aspect is of primary importance for infertility patients. In addition, as no electricity or heat production are involved in the resection process, there is a reduction in postoperative adhesion formations, leading to a faster recovery of the normal healthy endometrial layer. There are many techniques available for the surgical treatment of uterine malformations, but at present there is insufficient evidence to recommend the best corrective technique.
The additional use of the Shaver technique in a case of septum removal has not yet been reported. This case report shows that the combination of the Shaver technique with scissors could become the first-choice procedure to treat partial or complete uterine septa. The Shaver technique was able to remove all the thick endometrium, thereby allowing scissors to precisely cut the septum without bleeding and with the best possible visibility. In addition, the Shaver could remove all remnants of the septum to promote a regular and uniform endometrial healing. As clearly shown in our video, this method is a very fast, clear, precise, and safe technique to completely treat septa malformations. The Bigatti Shaver technique improves the quality of the result and reduces the risk of complications.